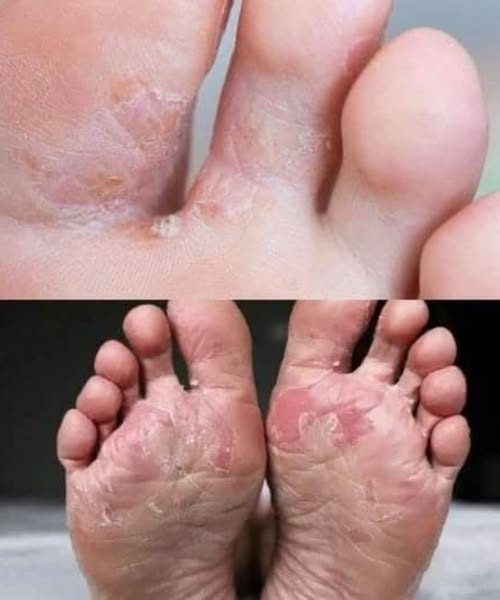
Diabetes, especially Type 2 Diabetes, can develop quietly over time, often without obvious symptoms in its early stages. Many people go months—or even years—without realizing that their blood sugar levels are elevated. During this time, however, the body may already be sending subtle warning signs. One of the most overlooked areas where these early signals appear is the feet.
The reason the feet are so commonly affected lies in how prolonged high blood sugar impacts the body. Over time, elevated glucose levels can damage blood vessels, reducing circulation, and impair the nerves—a condition known as Diabetic Neuropathy. Because the feet are farthest from the heart and rely heavily on proper circulation and nerve function, they are often among the first places where noticeable changes occur.
At first, these changes may seem minor or easy to dismiss.
One of the earliest signs can be persistent dryness in the skin. You might notice that your feet feel unusually rough, with cracked heels or flaking skin that doesn’t improve with regular moisturizers. While dry skin can have many causes, in the context of diabetes, it may be linked to reduced sweat production caused by nerve damage.
Discoloration is another important sign. Dark patches, redness, or uneven skin tone may indicate poor blood flow or underlying inflammation. In some cases, the skin may appear thinner or more fragile than usual. These visual changes are often subtle at first, but they can become more pronounced over time if the underlying issue is not addressed.
Numbness or tingling is one of the most commonly reported symptoms. Some people describe it as a “pins and needles” sensation, while others experience a complete loss of feeling in certain areas of the foot. This happens when nerves are damaged and can no longer transmit signals effectively. While it may not seem serious initially, numbness can be particularly dangerous because it reduces your ability to feel pain or injury.
This leads to one of the most concerning complications: unnoticed wounds.
Cuts, blisters, or sores that go unnoticed can worsen over time, especially when combined with poor circulation. Normally, the body heals small injuries quickly. But in people with diabetes, healing can be significantly delayed. A minor cut can turn into a persistent wound, increasing the risk of infection.
Slow-healing sores are a major warning sign.
If you notice that even small injuries on your feet are taking longer than usual to heal, it should not be ignored. This is often a sign that blood flow is compromised and that the body is struggling to repair tissue effectively.
Swelling, warmth, or redness can also indicate underlying issues. These symptoms may suggest inflammation, infection, or increased pressure in certain areas of the foot. In some cases, they can be early signs of more serious complications if left untreated.
Changes in nails and skin texture are another area to watch. Thickened nails, brittle edges, or unusual growth patterns may reflect poor circulation or fungal infections, which are more common in individuals with elevated blood sugar levels. The skin may also become either excessively dry or unusually shiny and tight.
What makes these signs particularly important is that they often appear before more widely recognized symptoms of diabetes, such as excessive thirst, frequent urination, or fatigue. This means that paying attention to your feet can provide an early opportunity for detection and intervention.
Early detection is critical.
The sooner diabetes or prediabetes is identified, the easier it is to manage and prevent complications. A simple medical evaluation, including blood tests, can determine whether blood sugar levels are within a healthy range. Catching the condition early allows for lifestyle changes and treatment that can significantly reduce long-term risks.
Daily foot care becomes essential, especially for those at risk.
This includes checking your feet regularly for any changes, washing and drying them carefully, and keeping the skin moisturized—but not excessively so between the toes, where moisture can lead to infections. Wearing comfortable, well-fitting shoes is also important to prevent pressure points and injuries.
Lifestyle choices play a major role as well.
Maintaining a balanced diet, staying physically active, and managing weight can help regulate blood sugar levels and improve overall circulation. Even small, consistent changes can have a meaningful impact over time.
It’s also important to understand that not every foot symptom automatically means diabetes. Many of these signs can be caused by other conditions, such as poor footwear, skin disorders, or temporary circulation issues. However, when symptoms persist or appear together, they should be taken seriously.
Ignoring early warning signs can lead to more severe complications down the line.
In advanced cases, untreated nerve damage and poor circulation can increase the risk of serious infections, ulcers, and, in extreme situations, the need for surgical intervention. These outcomes are often preventable with early awareness and proper care.
That’s why paying attention to small changes matters.
Your body often communicates in subtle ways before a condition becomes serious. The feet, though often overlooked, can provide valuable clues about what’s happening internally. Recognizing these signs early gives you the chance to act—not out of fear, but out of awareness.
In the end, staying informed and attentive is one of the most powerful tools you have.
By noticing unusual or ongoing symptoms and seeking medical advice when needed, you can take control of your health before complications arise. Protecting your feet is not just about comfort—it’s about safeguarding your overall well-being for the long term.